Pain Management Clinic
Doctors at American Pain and Wellness are dedicated to helping you with your pain in Allen, TX and Plano, TX. We specialize in back pain, neck pain, shoulder pain, joint pain and much more! For more information, please call us.


Introduction
At some time in our lives, the vast majority of us will experience the agony of pain. If you are lucky, your pain will be short lived. If not, you will have to do battle with the monster known as chronic pain. Some of us will quickly learn how to adapt to this monster. For others, the battle with chronic pain will result in unnecessary suffering, sleeplessness, hopelessness, sadness, financial hardship, and divorce.
For an individual suffering from chronic pain, it is difficult to see the light at the end of the tunnel. Many have seen multiple doctors and received endless treatments and yet still suffer from chronic pain. So what is the answer? Has modern medicine not yet discovered the magical pill or surgery to extinguish the pain? The answer is yes and no.
While our knowledge and treatments in medicine continue to improve, miracle treatments are rare. Many times we become over reliant on the medical system to fix our problems. When we visit the doctor to complain about a backache we are really trying to hand over our pain to the doctor and telling him to “fix me”. Unfortunately this type of belief becomes self defeating. In the endless search for the magical cure, visiting doctor after doctor, we overlook our most powerful tool-the ability of each one of us to effect our own health. One of the first steps in conquering pain is to understand the burden of your own pain and to decide to do something about it.
You’re not Alone – The Scope of the Pain Problem
It is estimated that as many as 30% of people living in the United States suffer from chronic pain. In fact, more than 50 million Americans are either partly or completely disabled by pain for a few days each month. Between the losses of 700 million working days a year, the cost of health care bills, compensation payments, and attorney’s fees, the price of pain soars to almost $100 billion a year.
Understanding Pain
In general, pain is divided into two categories, acute and chronic. Acute pain is temporary and usually results from tissue damage. Acute pain serves as an alarm system to warn us or protect us. We quickly pull our hand away from a hot stove to prevent us from burning our hand.
Acute pain can last from a few seconds to many months, but it generally goes away as healing occurs. Pain from a fracture, a burn, or an overused muscle is examples of acute pain.
Chronic pain is pain that simply doesn’t go away; it lingers long after the normal healing has occurred. It is triggered by trauma or a physical condition and persists although there is no ongoing tissue damage occurring. As opposed to acute pain, chronic pain serves no physiological or protective purpose.
Psychosocial factors strongly impact chronic pain. Everything from your upbringing and cultural attitudes toward pain, to your age, to previous experiences with pain impacts the intensity of your pain experience.
ACUTE PAIN
- Signals tissue damage or body dysfunction
- Has warning value
- Is short term. Goes away with natural healing or proper medical treatment
- Psychological factors less relevant
CHRONIC PAIN
- May or may not signal tissue damage or body dysfunction. In some cases is perpetuated by the brain.
- Has less warning value
- Persists for a long period of time. Keeps reoccurring despite medical treatment.
- Psychological and social factors often very important
How Pain Works
Biological Aspects of Pain – The role of the Nervous System
In most instances, painful sensations arise from tissue injury in the body. Sensitive nerve endings pick up pain signals and carry these messages along nerves to the spinal cord and then onto the brain. All along these complex pathways, there are biological “gates” that can be either opened or closed. When these gates are closed, pain is reduced or eliminated. When open, pain messages continue through the circuit. It is when these gates are jammed open that chronic pain cycles begin.
As you recall, acute pain is short lived and serves as a warning signal. When you fix whatever is wrong, the pain usually goes away. In the case of chronic pain, pain does not necessarily signal that the body is undergoing more damage. Most chronic pain is caused by a malfunction of the nervous system, either in nerves or the brain. The malfunction or opening of the pain gates causes and endless barrage of pain signals to cycle. Chronic pain then becomes a disease itself, taking on a life of its own.
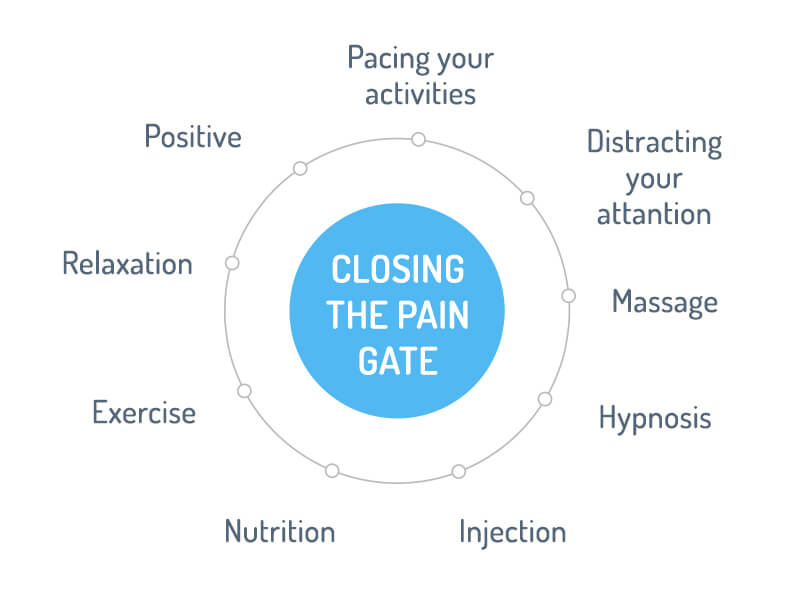
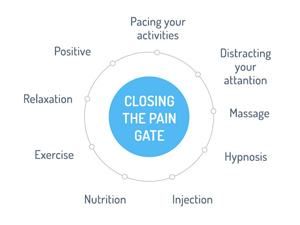
How can we close the gates of pain?
The gates are affected by several factors, most importantly by the pattern of nerve impulses which reach the spinal cord from the rest of the body, and nerve impulses coming from the brain. Sometimes the nerve impulses traveling through the spinal gates can be affected by other forms of physical stimulation. Giving your nervous system a competing source of input can fool the nervous system and alter your perception of pain.
There are many ways to accomplish this. You may have noticed that rubbing or massaging a painful area may have relieved your pain in the past. Applying electrical stimulation (e.g. TENS), applying heat or cold, acupuncture, or nerve blocks may also provide a competing source of input. It is also important to realize that certain mental activities or thoughts taking place in the brain can help to close the spinal gates.
Another way we can work to close the gates of pain is to affect the release of several chemicals that help pain signals travel to the brain. Neurotransmitters are biochemical messengers that carry pain signals from one nerve cell to the next. The three main neurotransmitters that send pain signals to the brain are substance P, NMDA (n-methyl-d-aspartate), and glutamate. Excess amounts of these chemicals, especially substance P, make it easier for pain signals to reach the brain.
Therefore, another way of stopping pain involves manipulating pain provoking neurotransmitters. This can be accomplished by prescription or over the counter medications, acupuncture, injections, hypnosis, or biofeedback. We will examine these techniques in greater detail in later chapters.
The role of the Endorphins
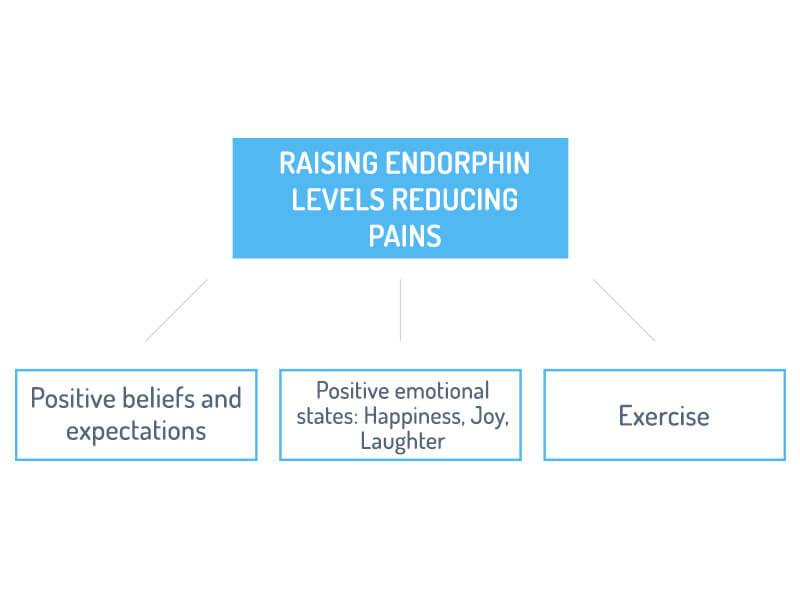
The endorphins are another class of chemicals which are produced in the brain and serve an important role in the pain experience. These chemical are naturally occurring pain relieving substances, similar to morphine or other opiates, produced in the body. Endorphins work on special receptor sites in the brain. They act as keys which unlock receptors thus generating nerve impulses to shut down pain. Morphine and other opiates have similar chemical structures which turn off pain.
Several situations or conditions raise endorphin levels in the brain thus reducing pain. They include thinking with a positive attitude, happiness, and regular exercise.
The Role of Stress
It is natural to connect a physical stress to the body, such a broken arm, to the perception of pain. The role of psychological stress may not seem as obvious. The brain structures involved in stress can affect the production of key hormones in the body, suppress the body’s immune system, and activate the autonomic nervous. These are the same biological changes that may occur from physical stresses on the body-the body may not differentiate between physical and psychological stress. The net effects of these changes on the body are to lower our internal resistance to pain, thus further encouraging the chronic pain cycle.
Many sources of stress feed into the chronic pain cycle. First off, as you would expect, pain itself is stressful. Pain sensations are perceived as undesirable and are at very least annoying. Pain creates tension, both physical and emotional. Physical tension may show itself as muscle tension or affect the cardiovascular, gastrointestinal, or immune systems. Emotional tension may reveal itself as anger, frustration, worry, depression, or frustration. Both physical and emotional tension, initially set in motion by pain, worsen pain. Thus the vicious cycle of pain is begins-pain leads to tension and tension leads to more pain.
A second source of stress comes from all the negative consequences that occur as a result of a chronic pain condition. Chronic pain may create difficulties with family relationships, social or recreation activities, self-esteem, and employment.
Yet another source of stress arises from the hardships that can be encountered from the stresses of everyday living. Everything from difficulties putting on your shoes in the morning to difficulties standing long enough to go grocery shopping are added on top of pain-related stressors. In the end, an individual not only suffers from chronic pain, but from chronic stress.
The consequences of chronic stress
Whatever the type of stress, either physical or psychological, the outcome on pain is to worsen it. Chronic stress also may result in other physical ailments such as tension headaches, muscle spasms, gastrointestinal problems, and elevated blood pressure. It can also lead to fatigue, depression, and a sense of hopelessness.
Fighting Back
Step 1: Accepting the Condition
The first step in controlling chronic pain is accepting that you have it. Chronic pain is a separate or at least an additional problem from the injury or disease that caused it. Remember, chronic pain is caused by a malfunction of the nervous system in which pain messages continue to be sent although ongoing tissue damage does not occur. Coming to grips with this is often difficult for individuals to understand, however, grasping this concept will go a long way in helping to develop coping mechanisms for chronic pain.
Accepting chronic pain does not mean you are accepting a lifetime of needless suffering. There are many treatments available to help reduce pain but you should not expect medications to relieve all of your pain or a procedure to completely solve all of your problems.
Accepting chronic pain does not mean you have to give up hope for the future. Although things may be difficult for you today, and you may not be able to see the light at the end of the tunnel, you should maintain hope for a better future.
Accepting chronic pain does not mean that you do not care about your situation. It does mean that worrying over your condition serves no purpose. Thinking that you’re going to live a life of misery will result in a self fulfilling prophecy-you will become a miserable person.
One beneficial coping mechanism is a “spiritual surrender”. This is the letting go of one’s useless efforts to control the unpleasant realities of life. Spiritual surrender is recognized by major religions, including Christianity and Judaism. Also, 12 Step Recovery Programs use this concept by reciting “The Serenity Prayer” at their meetings. The first verse reads:
“God, grant me the serenity to accept the things I cannot change, the courage to change the things I can, and the wisdom to know the difference.”
As the serenity prayer implies, you must accept those aspects of your chronic pain condition that cannot be changed. Focusing your efforts on aspects of your condition that you can change will take courage and wisdom.
The following sections describe many aspects of chronic pain that are under your control to change. How you incorporate these ideas into your daily life will affect the quality of your life. All it takes is the courage to change!
Step 2: Positive Thinking
Are you an individual who approaches difficult situations with great negativity or do you try to look at the bright side? Is your cup half empty or half full? Unfortunately, even the most positive and enthusiastic individuals tend to dwell on the negative when experiencing chronic, unrelenting pain. This type of pain can make the strong feel weak. It can cause logical thinkers to have irrational, distorted thoughts. These negative thought patterns reduce your ability to cope with pain. They lead to a distorted view of yourself and others. Irrational thoughts lead to needless stress and interfere in relationships.
This does not have to happen. Individuals who work hard at changing their attitude discover that their pain tolerance improves. You can take control of your pain instead of your pain taking control of you.
The Effects of Positive Thinking
- Increases happiness and well being
- Reduces pain
- Activates your healing system
- Relaxes your body and mind
- Increases confidence and self-esteem
- Increases your control over your pain
- Allows you to achieve more
Stopping Negative Thoughts
- Recognize and acknowledge your thought patterns in difficult situations. What does the situation mean to you? How are you reacting? What are your thoughts?
- Avoid negative “hot thoughts”. Hot thoughts are absolute demands. “I demand that they take care of this right now”. Hot thoughts are expressed in words or phrases like: must, never, always, needs to, ought to, and should have. Instead, ask how you can help yourself.
- Use problem solving strategies to cope with difficult situations.
- Use Affirmations/positive thoughts. Say to yourself, “Be calm, this will pass. I can do this.”
- Take deep breaths. Count to 10.
Step 3: Become Physically Fit – Use it or lose it!
Often individuals with chronic pain stop being active and proactive; they let pain rule their lives. This leads to loss of independence, loss of self esteem, and loss of self confidence. Inactivity leads to weakening of muscles, loss of flexibility, loss of stamina, and weight gain. These symptoms are known as physical deconditioning and disuse syndrome.
The following are consequences of prolonged physical inactivity:
- Muscle deterioration or atrophy
- Reduced joint flexibility
- Increase body fat in proportion to muscle mass
- Decrease resistance to infection
- Decrease in sex hormones and sex drive
- Reduction of brain chemicals, leading to increased depression
Exercise is one of the most important ways to fight back against chronic pain. The following body chemicals are changed by regular exercise.
1. Endorphins
Walking, swimming, stretching, yoga, Pilates, and gentle aerobics cause the release of endorphins which help lessen pain, fight depression, and improve self esteem.
Pain relief from exercise, in part, comes from the release of endorphins from the pituitary gland in the brain. Endorphins are ten times stronger than morphine. Even better yet, your body does not build up a tolerance to them as it would if you were taking pain pills. These natural opioids not only flood the brain, creating physical and psychological relief, but also work on closing the pain gates in your spine.
2. Serotonin
Exercise also increases the brain’s supply of serotonin. Serotonin, one the brains neurotransmitters, is one of pain’s worse enemies. In fact the mental exhilaration or “runners high” usually attributed to endorphin release, is probably more a result of increased serotonin release. Many researchers believe this because they know that serotonin has far greater effect on the mind than do endorphins which mainly affect the body.
3. Norepinerphrine
Although excess norepinerphrine release by the adrenal gland during extreme physical or psychological stress can actually jam the pain gates open, lesser amounts released during exercise will boost mood and energy. The net result is that norepinerphrine released during exercise will help fight pain.
As a patient with chronic pain, you may think there is no way you can safely exercise. But in reality, you can and should do some form of exercise to help yourself improve. There are some basic principles you must understand and incorporate into your exercise program.
Physical Exercise Programs: basic principles
- Find out your true physical limitations
- Live within your limitations
- Improve your activity tolerance/ Set Goals
- Improve self-acceptance
A. Recognizing True Physical Limitations
Discuss physical limitations with your health care provider. Ask for a referral for physical therapy. Take the time to learn your true limitations and the reasons behind them.
Many chronic pain sufferers limit themselves needlessly for a number of reasons.
- Fear and Avoidance. Learning about your condition and its limitations on your activities should alleviate unnecessary fear. As a chronic pain sufferer you must understand that hurt does not necessarily mean harm. Reasonable exercise will not break your spine or put you in a wheelchair.
- Distorted Thinking. You do not need to view activities as ‘all or none’. Thinking that “If I can’t do it the way I used to, I won’t do it at all” is self defeating. You need to make compromises in your approach to activities-pace yourself, take frequent breaks and find short cuts if necessary. Don’t give in or up!
- Secondary Gains. This is when you use pain as an excuse to avoid (or to gain) something based on your desires, not your true needs or limitations. An example of this is using pain as an excuse not to return to a job that you did not like in the first place. (Or avoiding exercise because you never did like it.) Stopping this behavior requires honest self examination.
- Physical Compensation or Overuse Syndrome. A natural reaction to pain is to overuse one body part to compensate for limited use of the painful body part. Limping, or using crutches because of pain may result in overuse of other body parts, resulting in additional pain. Excessive use of braces like those for the low back or neck will cause weakening of supporting muscles, thus leading to more pain. It is important to try to use as normal body movements as possible.
B. Improve Your Activity Tolerance
Take control by setting goals. First, establish a baseline for a particular activity. For example, measure how long you can walk or ride an exercise bike before provoking too much pain; be honest with yourself regarding how much is too much. Gradually and systematically increase your activity. Set small goals and keep a log to ensure success. For example, increase your walk or ride by one minute every 3 days or so as your tolerance improves.
Accomplishing your goal is extremely important. Do not stop every time you feel a small twinge of pain. If you know that the activity is not going to harm you, there is no reason to surrender to the pain. Admitting defeat is not the easy way out. You only succeed in opening the pain gates wider. You, in essence, allow your subconscious the approval to let pain through. Although it may be a struggle, you must take control and prove you are in charge by consistently improving your activity tolerance.
C. Living within Your Limitations
Learning your physical limitations is one thing but practicing them on a daily basis is another. Although some individuals know how far they can push themselves, they frequently find themselves doing too much and suffering afterwards. It is important to follow these principles:
- Strike a balance in activity; avoid too much and too little.
- Pace yourself.
- Use good body mechanics.
- Do warm up and cool down exercises
- Don’t let good days, enjoyable activities, or competition with others trick you into becoming careless and overzealous.
D. Improving self-acceptance
Regrettably, many individuals with chronic pain conditions suffer from low self-esteem. Inability to accept yourself and your limitations can lead to frustration, anger, stress, and depression. The following are some rules to help improve self esteem:
- A person with a physical limitation or disability is not less valuable than an able bodied individual.
- Think positively. Be thankful for what you have and what you can do.
- Channel your energy into skills that are not overly physically demanding.
- Do your best and be satisfied that you did so.
Accepting true physical limitations as defined by your healthcare provider and still challenging your body to improve its exercise tolerance is just one way you that can improve your condition and quality of life.
Step 4: Taking control of your pain through diet
In these days of modern medicine, we seek out the newest pill or procedure to magically cure our ailments. Too frequently we fail to recognize our own abilities to affect our health and wellness. We all know that a healthy diet, moderate exercise and eliminating smoking lessen our risk of heart disease and cancer. Did you know these same lifestyle choices affect pain as well? Yes, the cheeseburger and fries you ate yesterday did contribute to the exacerbation of your pain that ruined your sleep last night.
Most people, including doctors, don’t recognize the connection between diet and pain. Although Eastern medicine nutritional strategies have not been rigorously tested by governmental agencies, many ancient anti-pain nutritional strategies have helped individuals for thousands of years. Several generic strategies can help individuals with all types of pain problems including headache, back pain, or arthritis. The following are nutritional strategies recommended by Dr. Dharma Singh Khalsa, author of The Pain Cure:
1. Eat foods or nutrients that relieve inflammation.
Eating too much fat, especially the wrong types of fat such as animal fat, promote inflammation in the body. This is especially troublesome for individuals with chronic pain who eat a typical American diet high in poor quality fats.
Let’s examine why eating the right types of fat can control inflammation and pain in the body. Inflammation is controlled by several chemicals in your body, the most important of which are called prostaglandins. Prostaglandins are made from the fats we eat. In regards to pain, there are “bad” prostaglandins that promote inflammation and “good” prostaglandins that turn off inflammation in the body. Therefore, eating the right types of fat can help control inflammation and pain.
EPA or eicosapentaenoic acid is a “good” type of fat that comes from cold water fish, such as salmon, tuna, herring, mackerel, and sardines. It is also found in whole flaxseed or flaxseed oil. Eating two to five servings of fish per week or adding EPA supplements of fish oils or flaxseed oil helps with any pain control regimen.
Two other types of fats that help relieve inflammation are alpha-linolenic acid (ALA) and gamma-linolenic acid (GLA). ALA is found in vegetables, beans, fruits, and fish oils (salmon, tuna, and herring). It is also can be found in concentrated forms in flaxseed oil, canola, wheat-germ, and walnut oils. GLA is much rarer and can be found in borage oil, evening primrose oil, black currant oil, and hemp oil.
In addition to fats affecting inflammation in the body, several nutritional supplements are helpful with controlling inflammation as well. Turmeric, Boswellin, and Ginger are ancient botanicals that have been shown to reduce pain and inflammation in a similar manner to prescription anti-inflammatory medications.
Protein digesting enzymes including protease, bromelain, trypsin, lipase, pancreatin, and amylase have also shown been shown to have powerful anti-inflammatory effects. Several controlled studies have shown that these protein digesting enzymes provide pain relief from arthritic conditions.
Several antioxidant vitamins may also play a role in the management of pain and inflammation. Although vitamins A, C, E, and the mineral selenium don’t directly reduce inflammation, they serve to protect tissues that are overrun by inflammation.
Avoid animal fats and common cooking oils such as corn oil, safflower oil, sunflower oil, and sesame oil. Also, you should avoid processed and prepared foods that contain these fats and oils. You should also eat nonfat dairy products, such as fat free cheese, yogurt, milk, and sour cream. Make sure to check the labels! For a person with chronic pain, eating these fats is like pouring gasoline on a fire.
Anti-inflammatory Nutrients
HELPFUL
- Good fats-EPA,GLA,ALA oils
- Botanical-Tumeric, Boswellin, Ginger
- Protein Digesting Enzymes
- Antioxidant vitamins
HARMFUL
- Animal fat
- Common cooking oils-corn, safflower, sesame. Use olive oil instead.
2. Increase serotonin to raise your pain threshold
Serotonin, one of the brain’s calming neurotransmitters, plays a key role in an individual’s ability to control their pain experience. Raising serotonin has the following effects:
- Reduction of the pain promoting substance P. Substance P is secreted in your spinal column in response to pain signals from nerves and then carries pain signals to the brain.
- Serotonin decreases the release of substance P, thus helping to close pain gates.
- Blocks the perception of pain by modulating the intensity of pain signals within the brain.
- Improves mood, reduces fear, and relieves depression.
- Helps you fall asleep faster and stay asleep longer.
You can raise serotonin levels by practicing relaxation techniques, eating foods rich in the amino acid tryptophan (poultry, halibut, eggs, peanuts, cheddar cheese), taking the supplement 5-HTP (or 5-hydroxy L-tryptophan), or taking antidepressant medications such as Prozac or Zoloft.
3. Promote a healthy nervous system
Most of us were amazed to see Lance Armstrong battle back from testicular cancer and win the Tour de France. How did he overcome almost insurmountable odds? Was it luck? Was it divine intervention?
One thing that is certain is that his focus and determination guided him through his comeback. His journey required incredible “brain power” to overcome many obstacles.
You too use brain power in order to battle your chronic pain. The more powerful your brain gets, the better it will fight your pain. Improving brain power is accomplished in a variety of ways including utilizing physical and mental exercise, natural and pharmaceutical medicines, decreasing stress, and with nutritional therapy. This section will focus on nutritional methods of boosting brain power.
You already know that eating a diet high in animal fat and cooking oils increases inflammation. Did you know that eating a high fat diet literally rots your brain? Eating too much dietary fat, loaded with free radicals, speeds up oxidation in brain cells, causing them to die off. Every time you lose brain cells, you lessen your ability to fight off pain.
In addition to speeding up oxidation in the brain, excess dietary fat can clog small blood vessels in the brain. Impaired blood circulation, in turn, reduces the amount of oxygen and nutrients getting to the brain and lessens the brains ability to clear toxins. Eventually cell death occurs.
Eating a low fat, nutrient dense, balanced diet not only can boost mental energy, it can help you fight pain. Don’t eat empty calories of sugar and highly refined starches. You should eat foods that supply your brain and nervous system with the nutrients they need such as whole grains, vegetables, fruits, high-protein soy protein products, nonfat dairy products, and a variety of beans. Those of you who are not vegetarians, should eat only small portions of meat and several servings of cold water fish (like salmon and tuna) every week.
In addition to wholesome diet, several supplemented nutrients may be helpful in keeping your brain and nerves healthy. Pain fighting nutrients include:
- Vitamin A (10,000-20,000 IU daily), antioxidant properties protect brain cells
- Vitamin B Complex (50-100 mg daily), most important vitamin for nerves
- Vitamin C (3,000-6,000 mg daily), antioxidant for brain, needed to make neurotransmitters
- Vitamin E (400-800 IU daily), antioxidant that help protect the brain
- Magnesium (200-300mg), important for nerve function, deficiencies in migraine sufferers and fibromyalgia
- Selenium (50-100 mcg), antioxidant that can help some to feel more relaxed.
4. Avoid classic dietary pitfalls:
- Allowing yourself to overeat.
Although eating may become one pleasure a pain sufferer can still enjoy, excessive eating may undermine your anti-pain program. Not only does overeating disturb your hormonal balance and disrupt blood sugar levels, it worsens pain by placing more stress on muscles and joints of the body. - Allowing yourself to eat too little.
Under eating can starve your brain, nerves, and muscles of vital nutrients they need to fight pain. Eating too little can also trigger low blood sugar which can result in becoming more pain sensitive. - Allowing yourself to eat foods that trigger allergies and food sensitivities.
Certain foods may trigger pain responses in an individual by increasing levels of inflammatory other hormone-like substances called prostaglandins. Milk and dairy products commonly provoke pain reactions in many individuals with chronic pain conditions. As mentioned earlier, too much fat whether from dairy, meat or common cooking oils can elevate levels of inflammatory substances in the body. Cured meats such as bacon, hot dogs, ham, bologna, and cold cuts have preservatives and a myriad of other chemicals that can trigger allergic reactions. If you suspect food allergies or sensitivities you may need to see a nutritional health care professional and begin an allergy elimination diet. - Allowing yourself to eat foods that alter hormonal balance.
Hormones have a large impact on your thoughts, feelings, energy level, and perception of pain. The endocrine glands that have the most effect on your brain are your adrenal glands, your gonads, your pineal gland, and your pituitary. These glands produce the hormones adrenaline, cortisol, testosterone, estrogen, DHEA, and melatonin which affect your mind and mood. When you are healthy, they exist in a delicate balance.
After a period of illness, stress, and chronic pain, the balance is lost between your hormones resulting in depression, anxiety, lethargy, fatigue, diminished sex drive, and increased sensitivity to stress and pain.
Even though you may have chronic pain, you can still rebalance your hormones. The first step is to limit daily dietary fat. Eating too much fat stresses your liver, an important organ involved in maintaining you balance of hormones. Other foods which also stress the liver include sugar, chocolate, and alcohol.
To help promote liver heath, take abundant amounts of B vitamins and consider taking the herb milk thistle (or silymarin) 500mg-1000mg a day.
5. Stop Smoking
Several studies have linked smoking and a number of chronic pain conditions. A recent survey of 13,000 Britons found that smokers were significantly more likely to develop discomforting or disabling musculoskeletal pain than individuals that never smoked.
They found that, compared with those who had never smoked, current smokers had about a 50% higher incidence of reporting “pain in the past year preventing activity,” meaning pain so severe it precluded the individual from going to work or performing housework or hobby activities. Pain at all sites–lower back, shoulders, elbows, hands, neck and knees–was higher in smokers than non- smokers. What’s more, this association held even among respondents who had white-collar or other jobs that did not require heavy lifting or moving.
Why might smoking raise pain levels? Studies have suggested several explanations. First, the stimulant nicotine may affect the manner in which the brain processes sensory stimuli and heighten the perception of pain.
Second, smoking might cause damage to musculoskeletal tissues by reducing blood supply, raising clotting risks, or by reducing the flow of nutrients to muscles or joints.
Step 5: Practice Relaxation Techniques Daily
Pain and Muscle Spasm
Years of experience and research have taught us that with chronic pain comes muscle spasm. Muscle spasm is a reflex; it’s your body’s reaction to pain that you have no control over. Tense muscles can produce anxiety, depression, fear of more pain, bad posture, and immobility. Tension also causes headaches, indigestion, and palpitations. This muscle spasm serves no useful purpose in chronic pain.
Many individuals with chronic pain do not recognize that they have muscle tension because they have had pain for so long. There are those people with chronic pain who strongly believe they have no need to learn relaxation techniques, but nothing could be further from the truth. The only way to make a meaningful impact on tension is to practice relaxation techniques (this is not sitting on the couch in front of the T.V.!). The Benefits of Relaxation
Relaxation, the opposite of tension, has many benefits in individuals with chronic pain. Unfortunately it is not an automatic process and needs to be learned and practiced regularly to be effective. The beauty of relaxation techniques is that they can be used anywhere, at any time, and without the need to take a pill. The benefits of relaxation include:
- Relief of muscle spasm
- Release of natural pain relieving endorphins
- Reducing anxiety and fear
- Regaining a sense of control and confidence
Relaxation Methods
Several relaxation techniques exist, all with their advantages and disadvantages. The best technique for you is the one you feel most comfortable with. Relaxation techniques include:
- Controlled Breathing
- Progressive Muscular Relaxation
- Meditation
- Visualization
- Hypnosis
- Yoga
- Tai Chi
Controlled Breathing
This type of relaxation can help you cope with stressful situations or intense pain episodes. Position yourself either sitting or lying down with a straight spine.
- Take in a deep, comfortable breath through your nose while counting slowly to four. As you inhale, first fill the lower section of your lungs, then fill the middle part, and last fill the top. Feel your abdomen expand. Hold your breath for 3-4 seconds.
- Exhale slowly through your mouth. While you exhale say calming words such as “relax”, “easy does it”, or other words that suggest releasing of tension. As you exhale, feel your abdominal muscles contract and try to let your jaws, shoulders, and arms go limp.
- Continue for five minutes. If you become light-headed, alternate six regular breaths with six deep breaths.
Progressive Muscular Relaxation
Progressive Muscular Relaxation (PMR) was developed by Jacobson in 1939 and is widely used today. PMR uses the pendulum method – if you want the pendulum to swing in a particular direction, then you first have to pull it back in the opposite direction and then let go. In Progressive Muscular Relaxation, first you deliberately apply tension to certain muscle groups, and then you let go, and pay attention to how the muscles relax as the tension flows away. The aim is to work systematically through the body. Usually a person starts with the hands, working up to the shoulders, then works from the feet up to the shoulders again, leaving the face and neck for last. There is no reason to rigidly stick to a particular order, but it might be more difficult to start with areas in which physical and emotional tensions seem to concentrate, such as the shoulders, neck and face.
How to do Progressive Muscle Relaxation
There are two steps in the self-administered Progressive Muscle Relaxation procedure:
- Deliberately tensing muscle groups.
- Releasing the induced tension.
Tension-Relaxation Procedure
Step One: Tension – The process of applying tension to a muscle is essentially the same regardless of which muscle group you are using. First, focus your mind on the muscle group; for example, your right hand. Then inhale and simply squeeze the muscles as hard as you can and hold to the count of 5; in the example, this would involve making a tight fist with your hand.
Note: Beginners usually make the mistake of allowing muscles other than the intended group to tense as well; in the example, this would mean that there will be a tendency to tense muscles in your right arm and shoulder along with those of the right hand. With practice you will learn to make very fine discriminations among muscles; for the moment just do the best you can.
It’s important to really feel the tension. Done properly, the tension procedure will cause the muscles to start to shake. You might feel some intensifying of your pain but it should be within an acceptable range for you.
Note: Be careful not to hurt yourself, as compared to feeling mild pain. Contracting the muscles in your feet and your back, especially, can cause serious problems if not done carefully; i.e., gently but deliberately.
Step Two: Releasing the Tension- This is the best part because it is actually pleasurable. After the count to 5, just suddenly but gently let go. Let all the tightness and pain flow out of the muscles as you simultaneously exhale. In the example, this would be imagining tightness and pain flowing out of your hand through your fingertips as you exhale. Feel the muscles relax and become loose and limp, tension flowing away like water out of a faucet. Notice the difference between tension and relaxation.
Note: The point here is to really focus on the change that occurs as the tension is let go. Do this very deliberately. You are learning to make some subtle distinctions between muscular tension and muscular relaxation.
Stay relaxed for about 15 seconds and then repeat the tension-relaxation cycle. You’ll probably notice more sensations the second time.
Note: It is of utmost important to coordinate your breathing with the tension relaxation cycle. Every time you let go, exhale and feel the tension go out from the concerned muscle group along with the outgoing breath. The breathing must be relaxed and preferably abdominal. Muscle Groups
Here is an order that we find easy to remember which will help you not to forget any muscle group.
- Hands: Clench the fists.
- Arms: Tighten biceps and lower arms together, without the hands.
- Shoulders: Inhale, hold your breath and raise your shoulders as if to touch your ears.
- Feet: Screw up your toes.
- Front of legs: Point your foot away from you so that it is almost parallel with your leg.
- Back of Legs: Flex your feet upwards, stretching your heels away from your body.
- Thighs: Tighten them while pressing your knees down into the floor. Pull your knee caps to your hips.
- Bottom: Clench your buttocks together.
- Stomach: Hold your stomach muscles in tight.
- Lower Back: Press the small of your back into the floor.
- Chest: Breath in, hold your breath, and tighten all your chest muscles.
- Shoulders: Breath in, hold your breath and raise your shoulders as if to touch your ears.
- Neck:
- Stretch your head up, as if your chin could touch the ceiling.
- Bend your head forward until your chin reaches your chest.
- Mouth and Jaw: Press your lips together and clench your teeth.
- Eyes: Close them up tight.
- Forehead and scalp: Raise your eyebrows as if they could disappear.
- Face: Screw all the muscles up together.
After learning the full PMR procedure, you will spend about 10 minutes a day maintaining your proficiency by practicing a shortened form of the procedure. But in the beginning it might take longer and it would be a good idea to tense and relax one limb at a time instead of both together. With time and practice, approximately 3 to 6 weeks, you may shorten the exercise gradually. For example, you could try collapsing some of the muscle groups until you only work on your arms, legs, abdomen, chest and face. Ultimately, you will acquire something that will probably become an indispensable part of your daily life, and the initial drudgery of practice will be long-forgotten.
Recommendations:
It is recommended that you practice full PMR twice a day for about a week before moving on to the shortened form. Of course, the time needed to master the full PMR procedure varies from person to person.
Here are some suggestions for practice:
- Always practice full PMR in a quiet place, alone, with no electronic distractions, not even background music.
Remove your shoes and wear loose clothing. - Avoid eating, smoking, or drinking. It’s best to practice before meals rather than after, for the sake of your digestive processes. Never practice after using any intoxicants.
- Sit in a comfortable chair if possible. You may practice lying down, but this increases the likelihood of falling asleep.
- If you fall asleep, give yourself credit for the work you did up to the point of sleep.
- If you practice in bed at night, plan on falling asleep before you complete your cycle. Therefore, consider a practice session at night, in bed, to be in addition to your basic practice.
- When you finish a session, relax with your eyes closed for a few seconds, and then get up slowly. (Orthostatic hypotension-a sudden drop in blood pressure due to standing up quickly-can cause you to faint.) Some people like to count backwards from 5 to 1, timed to slow, deep breathing, and then say, “Eyes open. Supremely calm. Fully alert.”
Give PMR a try! It only takes a few minutes out of your day; and the rewards of enhanced recovery, better muscle control and the ability to more effectively manage stress are well worth the investment.
Disclaimer: If you continue with this procedure, you do so at your own risk. American Pain and Wellness cannot be held responsible in any way for any consequences arising out of practicing Progressive Muscular Relaxation. The information given is strictly for personal use.
Step 6: Understanding Thoughts, Feelings, and Actions as they relate to Pain
The experience of pain is a complex event, involving an interaction between our physical state-nerves, the brain, and body chemicals-and our psychological state–our thoughts, attitudes, and history.
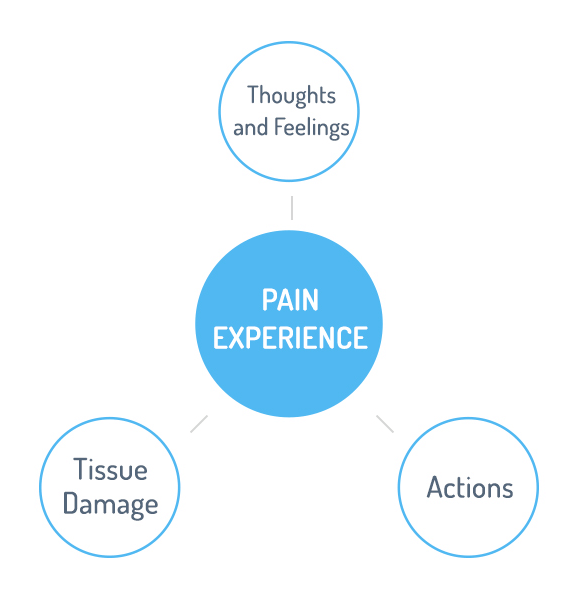
A person who focuses on the details of their pain often imagines that they have every last disease under the sun, stops seeing friends, thinks the future is bleak and will therefore suffer to a greater degree than someone who has more rational thoughts and actions.
Those individuals who keep a positive attitude and preoccupy themselves with things other than their pain tend to suffer less. They can, in effect, close pain gates by possessing positive thoughts and taking on healthy actions. Identifying Distorted Thinking
It is difficult to identify irrational thoughts during times of emotional or physical stress. If you find yourself frequently nervous, tense, depressed, feeling hopeless and angry your thinking is likely distorted. Your perception of pain has probably become unrealistic. For example, if you experience pain from degenerative disc disease, you may be convinced you will end up in a wheelchair. While you may not be imagining the medical problem, you are not putting the facts into proper perspective.
Distorted thinking occurs in many forms, including:
- Filtering: You focus on the negative aspects of a situation, ignoring all of the positives.
- Catastrophizing: You think the worse is going to happen. You picture horrible outcomes.
- Overgeneralization: You come to a conclusion based on one piece of evidence. If something bad happens once, you expect it to happen every time.
- All or None Thinking: Things are black and white with no middle ground. “I had a bad experience trying to ride an exercise bike Monday, therefore all exercise is bad”.
- Magnifying: You make the problem greater than it really is.
- Selective Attention: Focusing on threatening signs, rather than paying attention to positive signs.
- Over interpreting ambiguous signs: Thinking a sign or symptom has awful consequences. For instance, interpreting weakness in the back as a sign of worsening degeneration rather than acknowledging it is from a lack of exercise.
- Personalization: Thinking that everything other people say or do is in reaction to you.
Changing Distorted Thinking
Once you begin to study yourself and your thought patterns, you can change your negative thoughts by using positive alternatives. For example, instead of thinking, “I am not going to be able to work because of my back pain” think “It may be difficult, but I can continue to work. I will have to pace myself, but I can still work”. These types of positive coping statements can help you master your pain and cope with challenges.
On the other hand, being overly enthusiastic may set you up for failure. Statements such as, “Pain doesn’t affect me, I can work just as hard as I ever could” are unrealistic. Confidence plays a large role in managing pain. Don’t set yourself up for failure by denying the effect pain has on your abilities. If you prepare for challenges, you will better position yourself for success. And if success does not come right away, you will not feel so overwhelmed.
Feelings
Feelings also contribute to your pain experience. It is very common for individuals who suffer from chronic pain to feel depressed or angry. In some cases, depression may have existed before the pain condition began. Regardless of which came first, depression makes the pain experience much worse: it lowers pain tolerance and makes it difficult to cope with pain.
In order to treat depression, you must first recognize it. Common symptoms of depression include:
- Feelings of sadness
- Tearfulness
- Feelings of hopelessness
- Feelings of guilt
- Feelings of failure or self-blame
- Decreased pleasure in activities you used to enjoy
- Irritability, frustration
- Deceased energy levels
- Difficulty sleeping or excessive sleeping
- Decreased appetite or excessive appetite
- Decreased interest in sex
- Thoughts of suicide
Take action against depression
- Breaking free of depression is not easy. Chronic pain can cause depression, and depression can worsen chronic pain. It is important to recognize this connection and take steps to fight depression at the earliest signs.
- Become aware of and change distorted thinking. Depression always distorts your thinking.
- Talk to a trusted friend, religious leader, or professional counselor. Let them give you feedback on your altered thinking.
- Try to keep up with your daily responsibilities as best as possible, even if you don’t feel like it.
- Exercise: take a walk. Remember, exercising raises natural pain killing substances called endorphins which help close the pain gates.
- Interact with other people, whether it’s meeting a friend for lunch or a walk, joining a chronic pain support group, or taking a class.
Try to think of all of the things you can be grateful for in your life. Count your blessings! - See your doctor to consider antidepressant medications.
- Do not treat mental pain with alcohol or non prescription drugs as these interact with prescriptive medications and can cause irreparable harm to your organs.
Anger
Many individuals with chronic pain experience problems with anger. Although anger can distract you from your pain, it has many negative consequences. Anger affects your health-increasing blood pressure, worsening digestive problems, triggering headaches, and setting off muscle spasm.
Anger and aggressive behavior harm your relationships. It frequently results in conflict, alienation and isolation.
Anger can trigger a vicious cycle– aggressiveness or hostility may generate an aggressive or hostile reaction directed back at you. This in turn fuels the fire, adding to your own anger and rage.
Anger Management
Controlling anger requires an individual to recognize that his or her thought pattern is irrational. Examples of anger triggering beliefs include:
- You should not, must not treat me this way.
- How terrible for you to have treated me so wrongly.
- You are an awful person for behaving towards me that way.
The first step in anger management is to admit that you are angry.
Second, you must take responsibility for your anger. Angry individuals tend to externalize their anger and blame others for their problems. Try to remember that only we make ourselves angry.
Third, challenge your thought patterns that trigger anger. Does blaming someone else help you get what you want? Is anger going to help take away your pain and suffering? Probably not. Blaming others or feeling like someone owes you, either medical treatment or disability compensation, are road blocks to recovery. The anger from these feelings can fester until it consumes your thoughts, and prevents you from focusing on constructive ideas and actions.
Constructive thoughts and actions to control anger
Coping Thoughts
- Stay calm; I’m not going to let them anger me.
- Take a deep breathe and relax-I’m in control.
- I can stay calm and relaxed.
- Easy does it; getting mad won’t help.
- It’s not worth getting angry about.
- There is no reason to take my stress out on others.
- Recite the serenity prayer.
Constructive Actions
- Identify and change your distorted thoughts.
- Use humor and laughter.
- Distract yourself with recreational activities or a hobby.
- Learn to accept things you cannot change.
- Use relaxation techniques.
- Talk to a professional counselor.
- Join a pain support group.
- Exercise regularly.
- Listen to music.
- Use prayer.
Step 7: Establish Regular Goals to take control of your pain.
Setting realistic goals is an essential step in taking control over your pain. It is important to set regular targets in order to achieve results. Make your targets simple and realistic-something you know you can accomplish. Being too optimistic and setting your goals too high will result in failure. Failure may trigger fear and depression.
Set short and long term goals. If you would like to return to work within three months, identify what going back to work will entail. Will you have to stand for 4 hours or sit for 8 hours? Achieve your long term target by accomplishing short term goals along the way.
The secret to successfully accomplishing your goals is to challenge yourself without crashing and burning. By gradually pushing yourself to accomplish new goals, you will improve your quality of life and your self-esteem.
These are a few examples of goals individuals may wish to work on.
- Decrease my reliance on pain medications.
- Improve my general health through exercise and diet.
- Improve my attitude.
- Practice regular relaxation techniques.
- Find more ways of distracting my mind away from focusing on pain.
- Find more effective ways of dealing with my anger.
- Improve my relationships with friends and family.
- Find a job that is more compatible with my physical limitations.
- Seek help for feelings of sadness, depression, or hopelessness.
Step 8: Get people to treat you the right way.
Although people with chronic pain may not be aware of it, they either directly or indirectly send out signs that seek out attention from others. It may be a groan, a limp, or pained facial expression that tells others things are not well. Your subconscious may be broadcasting signals in order to receive sympathy and attention.
Unfortunately, if you’re trying to break free of pain’s grip controlling your life, broadcasting your pain can be self-defeating. Family or friends usually react to your responses in two manners-both of which can be unhealthy.
First, they can become unsympathetic and pay no attention to your signals, depriving you of attention and believing you are not in pain. Or, perhaps even worse, they may become too caring, doing every task for you, making you feel like you have little self-worth. Sometimes a spouse or other family member takes complete control over the medical care of the individual with chronic pain. He or she may take the individual from doctor to doctor, seeking a medical cure. He or she may do all the speaking for the individual, eroding the pain sufferers pride, confidence, and self-esteem.
Families of chronic pain sufferers must strike a balance between ignoring the chronic pain sufferer’s signals for attention and trying to do too much for them.
Guidelines for how to treat a family member with chronic pain include:
- Encourage the individual with chronic pain to become as active as possible. Try not to focus on the individual’s pain. For example, do not ask them, “How are you feeling today?” These types of questions may only serve to remind them that they have pain.
- If the family member is constantly focused on his or her pain, try to distract them with interesting activities. Try to encourage looking at the bright side of things, encourage exercise, or relaxation techniques.
- Try to encourage independence whenever possible. Don’t try to do too much for the individual-it will only hurt their self-esteem and make them feel like an invalid.
How you act makes a difference
It is important to recognize that the way you act has a large effect on others. If you act as “poor pitiful me”, you will be treated as “poor pitiful little old you”. In turn, you will think less of yourself as an individual, creating more negative and irrational thinking, and thus opening your pain gates even further.
If, on the other hand, although you may hurt, you at least come across as positive, you will be accepted as normal. For example, if someone asks, “How are you?” and you reply “terrible, my back is killing me”, the person may become nervous about interacting with you. He or she may, in fact, try to avoid you in the future. If, however, you say “Great”, although you may not feel this way, you are at least helping to cope with your situation. Others will engage you as an equal and not as an invalid. You will maintain your self-respect and confidence.
Become self reliant to build confidence and self-esteem.
It is natural as a pain sufferer to need to feel good about yourself and the surroundings you find yourself in. Unfortunately, you cannot always place yourself in a supportive, comfortable atmosphere. People may not always treat you with kindness and understanding. Therefore, it is important for you to build self-confidence, and not rely on others for the way you feel about yourself. You need to be able to feel confident about yourself regardless of whether someone looks at you funny or someone says something not so nice. Confidence and self-esteem go hand in hand to boost your self-image and your relationships with others. They allow you to ask for that pay raise or go on that job interview although it may not work out favorably.
Get rid of avoidance behaviors
Do you ever use pain as an excuse to get out of something you don’t like doing? You must become aware and eliminate these types of defeating pain behaviors. Using pain as an excuse will act as a road block, preventing you from taking control over your pain.
Robert used his back pain as an excuse to avoid having to sit for a two hour drive to his mother and father in-laws. At the time, Robert didn’t consciously realize that he used his back pain as an excuse not to visit his in-laws, an activity he did not care for. The next weekend, a buddy of Robert’s called to ask if he would like to join them for a day of fishing at the lake. When Robert’s wife asked him if he could tolerate the car ride, he had to hesitate and think. He eventually declined to go on the fishing trip after realizing his pain tolerance should theoretically not be different for activities he disliked versus those he liked.
Robert would have been better off being more honest with himself and his wife. Perhaps he should of said “If I am going to suffer increased pain from a car ride, I would rather make it worse doing something fun”. Doing an activity that he enjoyed may have helped his attitude even though it may have worsened his pain.
Sex and Pain
We have all heard the saying “not tonight honey, I’ve got a headache”. Although it is certainly possible for a person with pain not to feel well enough to become intimate, using pain as an excuse may have other meanings. It may indicate that you feel that your partner needs a bath; I’m mad at you for not taking out the garbage; I’m afraid I’m not attractive to you anymore; or I’m worried I can’t perform sexually anymore.
Whatever the real reason is for not having sex, the person with chronic pain needs to be honest about the real reason for not engaging in sex. Talk with your partner. Work out your concerns. Although sexual activity can be uncomfortable for pain sufferers, most individuals feel it is important in a relationship. Without intimacy a man may feel less masculine or a women less feminine. Sex can keep you connected with your partner while making you feel as if you are in command of your life and not your pain.
Step 9: Working with your doctor
Suffering from pain can leave you irritable and frustrated. If you want to develop a good relationship with your doctor and his office, remember not to take out your frustration on your physician or his staff. Your doctor’s office is more likely to be responsive if you act respectfully rather than combative with demands.
Your doctor has a limited time to evaluate your problem and discuss treatment options. Therefore, come on time to your appointments and make sure to fill out all paperwork as requested by the office. Try to organize your thoughts prior to your visit so that you can communicate your problem in a concise manner.
When you talk to your doctor about treatments, don’t expect him to have a quick fix for you. Chronic pain is a complex problem in which many require several treatment forms. Chronic pain may need to be treated just like other chronic medical conditions. Just like a diabetic needs to receive ongoing treatment, a chronic pain patient may require long-term treatment.
Medications:
Several medications are used to treat chronic pain. The main categories of medication used to treat chronic pain include:
- Simple Analgesics. These mild pain relievers can control pain without causing drowsiness. Several of these medications are available without a prescription– they include acetaminophen, aspirin, and nonsteroidal anti-inflammatory medications such as ibuprofen.
- Adjuvant Analgesics. Adjuvant analgesics are medications that are used to treat conditions other than pain. However, because of the way these medications work, they can also reduce pain.
- Multipurpose analgesics such as anti-depressants or corticosteroids.
- Analgesics for neuropathic pain (nerve pain) such as local anesthetics or anticonvulsants (Neurontin, Gabapentin).
- Analgesics for musculoskeletal pain such as muscle relaxants (Robaxin, Soma, Flexeril)
- Opioid Analgesics. These narcotic drugs, either derived from opium or synthetic opiate can alter a person’s mood and behavior. Opioid analgesics have the potential for addiction in some individuals. These medications include Hydrocodone, Morphine, Oxycodone, and Methadone.
Opioid Analgesics and chronic pain.
Opioid medications work by reducing pain by affecting receptors in the brain and spinal cord. Adjuvant non-opioid medications, in contrast, tend to work more specifically on injured body tissues. Opioids decrease the brain awareness of pain, whereas non-opioids alter tissue chemicals at the injured body site by reducing inflammation or decreasing the pain threshold.
Although opioids are stronger pain relievers than adjuvant analgesics, they may have several pitfalls. An individual taking opioid pain relievers may develop tolerance, physical dependence, and more rarely addiction. Tolerance is characterized by an individuals need to increase the dosage of opioid over time to produce the same pain relieving affects. Dependence means that over a period of time your body has become dependant on the medication-if you stop it abruptly, you will go through withdrawal. Addiction on the other hand refers to a person taking pain medication for the “high” effect. Addiction is characterized by loss of control, compulsive drug use, and continued use of drug despite its harm. Individuals who develop tolerance and dependence to opioids do not necessarily become addicted to pain medication. In fact, the vast majority of individuals taking pain medication for a chronic pain condition do not develop an addiction.
Opioids are commonly used for pain control for conditions causing pain for a limited period of time such as after surgery or breaking a bone. As the body heals, the pain medication is tapered until the person if off pain medication. In some cases opioids are used to treat cancer pain or pain related to other terminal illnesses. In these situations issues of dependency or addition are not a concern.
Opioids and non-malignant pain: the double edged sword
Although several individuals in the field of medicine feel that pain is under-treated in many individuals, there remains a controversy over the use of opioid medication in chronic non-malignant pain. Non-malignant pain is defined as pain that is not caused by cancer or a terminal illness.
Some doctors feel that opioid medications, which produce an automatic physical and psychological dependence, should not be used for chronic pain treatment because they have a potential for addiction. They also argue that opioids should not be used to treat non-malignant pain because they can change an individual’s mood or behavior. Another concern is that individuals that take opioids regularly may develop a strong belief that if they don’t take pain medications they will be overwhelmed by pain. Fear creates a psychological need to continue to take pain medication.
On the other hand, other doctors contend that many individuals with chronic debilitating pain can take opioid safely without problems. People can take pain medications on a regular basis, just as a diabetic patient takes insulin to treat their disease process. They become more functional, re-enter the work force, join in activities with their families, and report better control of their pain while taking opioid medications. Many of these individuals do not need to increase their dosages of medication. They lead relatively normal lives.
So where does that leave us? Is it reasonable to take opioids for non-malignant pain? It is this author’s feeling that opioid can be used safely to treat chronic non-malignant pain. The ultimate decision is up to the individual with the chronic pain condition and his or her physician. Needless to say, there are many other issues to consider when taking pain medications for a chronic pain condition. One of the strongest concerns is addiction. The following are red flags raising the concern over psychological dependence and addition. Please consult your physician with any of the signs below.
Signs of psychological dependence and addictive behavior
- Do you use pain as an excuse to take opioids when you want to forget your troubles?
- Do you think you are taking more pain pills than you should?
- Are you taking more medication than your doctor has prescribed?
- Do you use excuses to get prescriptions early such as “I lost my medication”, “My medication was stolen”, and “I dropped my medication into the drain”?
- Do you get pain medication from more than one doctor? (Do you doctor shop?)
- Have family members expressed concern over your behavior or the amount of opioid you are taking?
- Have you become physically or psychologically abusive to a spouse or other family member?
- Do you try to obtain opioids illegally or take pain medications prescribed for someone else?
- Have you become forgetful or lose track of hours or days because of taking opioid pain medications?
Step 10: Putting it all together
Taking control over your chronic pain is not easy. In fact, it may be one of the most difficult challenges you face in your lifetime. Some individuals will never take control over their pain because they expect that their doctor can and should take it all away. They don’t take responsibility to change their thoughts and behaviors so that their pain can be controlled. Some individuals will eventually take action to control their pain only to relapse into the same poor habits they previously broke. Others will practice self- management techniques on a daily basis and conquer the chronic pain beast.
Here is a summary of key points discussed in earlier sections on this website.
- Acknowledge that you have pain.
The sooner you accept that you have a pain problem, the earlier you can focus your energy on healing. Constant complaining to your family and friends is not going to help you and will only remind you of your pain. This does not mean that your pain is not real or that you are not suffering. It also does not mean that you should not seek help from your doctor. - Use positive thinking.
Individuals with chronic pain, who work to change their attitudes, and make the most of their situation, will discover that their tolerance to pain improves. Eliminating irrational thoughts will help lessen stress and will allow an individual to cope more healthily. Positive thinking closes the pain gates, increases happiness and well being, increases confidence and self-esteem, relaxes your body and mind, and activates your healing systems. - Exercise-Use it or lose it!
Having chronic pain does not mean you should become a “couch potato”. An initial increase in pain with exercise does not necessarily mean harm. Reasonable increases in activity or exercise are usually beneficial to those with chronic pain conditions. Benefits of exercise include release of natural pain relieving substances called endorphins, muscle strengthening, improved joint flexibility, increased muscle mass and reduced fat, reduction in depression, improved immunity, and improved self-esteem. - Use diet to help control pain.
- Eat foods that relieve inflammation. Eat the two types of fat that relieve inflammation, alpha-linolenic acid (ALA) and gamma-linolenic acid (GLA). ALA is found in vegetables, beans, fruits, and fish oils. It can also be found in concentrated forms in flaxseed oil, canola, wheat-germ, and walnut oils. GLA is much rarer and can be found in borage oil, evening primrose oil, black currant oil, and hemp oil. Avoid animal fats and common cooking oils such as corn oil, safflower oil, sunflower oil, sesame oil. These types of fats cause our bodies to release chemicals that promote inflammation (arachodonic acid). For a person with chronic pain, eating these fats is like pouring gasoline on a fire.
- Elevate serotonin levels. Raising serotonin levels reduces your perception of pain, improves mood, helps regulate sleep cycles, and reduces levels of substance P, the main pain promoting chemical in the body. You can raise serotonin levels by eating foods rich in L-tryptophan (chicken, halibut, eggs, peanuts, cheddar cheese), taking the supplement 5-HTP (or 5-hydroxy L-tryptophan), or taking antidepressants such as Prozac, or Zoloft.
- Identify food sensitivities that worsen pain. In some individuals, various foods may trigger release of inflammatory chemicals in the body, thus worsening pain. Possible culprits may include milk and dairy products, corn, cured meats (bacon, hot dogs, bologna, and ham), eggs, citrus fruits, potatoes, tomatoes, nuts, coffee, wheat, oats, or rye. Keeping a food and pain diary will help you identify any sensitivity that you may have.
- Practice relaxation techniques daily.
Relaxation methods such as progressive muscular relaxation, meditation, visualization, hypnosis, yoga, or tai chi can help control stress, tension, and pain. Just like most things in life, the more you practice, the better you become at them. Relaxation techniques must be practiced regularly in order for them to be effective. - Understand how thoughts, feelings, and actions connect to pain.
The experience of pain is a complex interaction between our nerves, brain, body chemicals, and our psychological state. Distorted or pessimistic thoughts can lead to increased pain and suffering. Recognizing the troubled thoughts and replacing them with constructive alternatives is vital.
Chronic pain and depression feed on one another. Chronic pain can cause or worsen depression and depression can worsen chronic pain. Adequate treatment of depression is an important part in gaining control over chronic pain. Combating depression may involve exercise, counseling, and treatment with antidepressant medications. - Take control of your pain by setting regular, realistic goals in life.
Just as the old cliché says, “you must walk before you can run”, taking control over pain requires setting small regular goals. For instance, if you would like to return to a job which requires that you stand for most of the day, you may have to set targets of standing for 15 minutes at a time, then progress to 30min, and then to one hour and so on. The key is to create a balance between challenging yourself to accomplish new goals without setting yourself up for failure. By gradually pushing yourself to succeed in new goals, you will improve your pain tolerance as well as improve your self-esteem. - Get your family to reinforce helpful actions-not the “poor pitiful me” behavior.
If others constantly treat you as if you are disabled, you will be conditioned to feel and act as an invalid.
We serve patients from Allen TX, Plano TX, Fairview TX, McKinney TX, Parker TX, Lucas TX, Murphy TX, Frisco TX, Richardson TX and Collin County Texas.